Session Information
Date: Thursday, March 19, 2026
Title: Plenary Abstract Session I
Session Time: 2:45PM-3:00PM
Background/Purpose: Despite treatment advances and continued quality improvement efforts, outcomes for our patients with juvenile idiopathic arthritis (JIA) remain suboptimal. To address this challenge, we partnered with Integrated Care Solutions (ICS), our hospital’s population health management subsidiary, on a chronic condition value-based care program. The program aim is to transform the way specialty services are delivered by supporting care models that promote high quality, cost-effective specialty care that encourages care coordination and reduces ineffective, preventable, and inappropriate treatments for ICS’s 240,000 value-based pediatric lives. This project reviews cost data for patients with JIA under an ICS value-based agreement as this information is needed to identify a cost measure to fully advance value-based care.
Methods: Cost data for the entirety of health care costs were analyzed for patients with JIA that had active eligibility in an ICS health plan for the duration of the 12-month period from July 2024 to June 2025. Cost data was broken down into the following categories: prescriptions, physician (e.g. office visits), hospital outpatient (e.g. emergency department visits, radiology services), hospital inpatient, ancillary (e.g. mental health services, durable medical equipment), and dental. Detailed prescription data was analyzed including medication name and paid amount.
Results: We analyzed cost data from 176 patients. Cost by category is highlighted in Table 1 with the total cost of care being $5,044,838 (average of $28,664 per patient). A majority of costs (61.1%) are from prescriptions with ‘hospital inpatient’ (15.5%) and ‘hospital outpatient’ (14.3%) being the next 2 most costly categories. $2,832,814 of prescription costs (91.9%) are related to the rheumatology medications listed in Table 2 with 1252 prescriptions (average 7.1 prescription per patient per year; average 104.4 prescriptions per month). Adalimumab has the most prescriptions (313; 25%) and far exceeds any other medication in cost representing 62.11% of all prescription costs and 37.94% of the entire cost of care for all JIA patients. An adalimumab biosimilar prescription averages 27.27% of the cost of adalimumab-originator.
Conclusion: Prescriptions were the highest category of the cost of care for our JIA population. Furthermore, costs from one single medication – adalimumab – largely drove this overall cost. We plan to initiate a cost metric in 2026 related to increasing adalimumab biosimilar use to improve costs while not sacrificing the quality of care provided to our patients with JIA to advance value-based care.
Table 1. Cost of care for patients with JIA.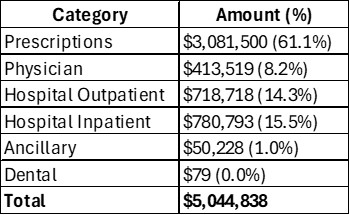
Table 2. Prescription cost data for patients with JIA.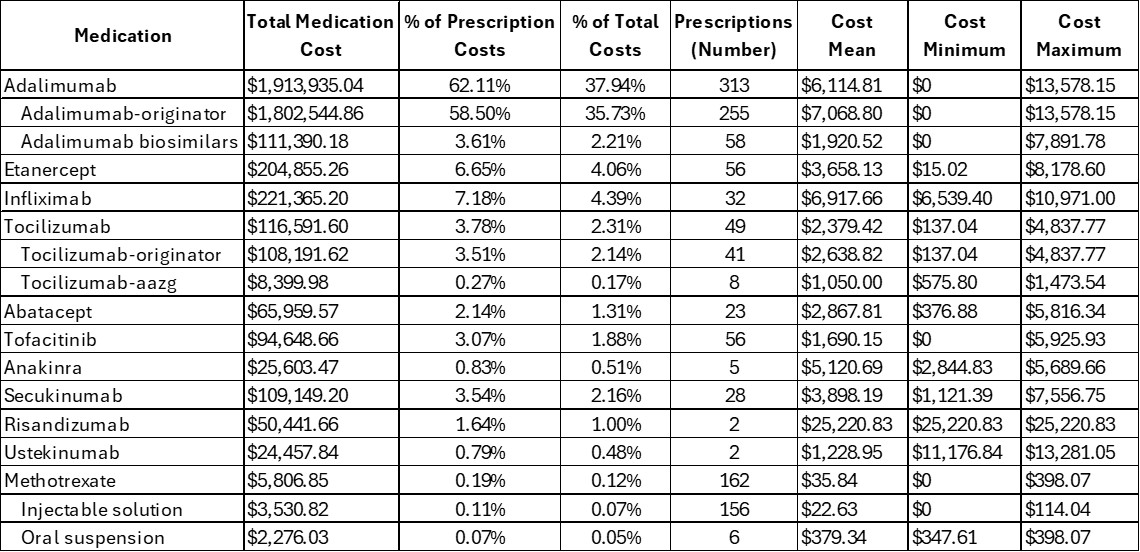
To cite this abstract in AMA style:
Harris J, Harris L, Diederich K, Moran R, Fox E, Favier L, Quinn S, cooper a. Assessing Juvenile Idiopathic Arthritis Healthcare Costs to Advance Value-Based Care [abstract]. Arthritis Rheumatol. 2026; 78 (suppl 3). https://acrabstracts.org/abstract/assessing-juvenile-idiopathic-arthritis-healthcare-costs-to-advance-value-based-care/. Accessed .« Back to 2026 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/assessing-juvenile-idiopathic-arthritis-healthcare-costs-to-advance-value-based-care/
