Session Information
Session Time: 5:00PM-6:00PM
Background/Purpose: Pediatric Systemic Lupus Erythematosus (SLE) is a chronic autoimmune disease with multi-system involvement and diverse clinical manifestations, typically presenting with greater severity compared to adult forms. Early recognition and improved treatment are essential for clinical and disease management. This project characterizes the clinical manifestations and rheumatological biomarkers of pediatric SLE over time.
Methods: Retrospective cohort study of 181 patients diagnosed with SLE between 2018 and 2022 at a tertiary care children’s hospital rheumatology clinic. Clinical and biochemical disease status were evaluated at baseline, 6, 12, and 24 months and following stratification by pre- vs post-pubertal (age ≥ 12) onset. Chi-square testing was used to compare prevalence of symptoms and biochemical abnormalities and to identify associations between biochemical abnormalities and clinical manifestations.
Results: The cohort had a mean age of 13.7 years (SD 3.2); 86% were female. 58% were White, 27% Black, and 49% Hispanic/Latino (Table 1). 28% of patients had pre-pubertal onset. 99% of patients had positive ANA and 65% had dsDNA antibodies. The most prominent cutaneous manifestations were malar rash (47%) and oral ulceration (31%), which was more frequent in post-pubertal presentation (35 vs 20%, χ2 = 4.3, P = 0.04). Joint involvement occurred in 44% of patients and more often post-pubertally (49% vs 31%; χ²=4.7, P=0.03). Lupus nephritis occurred in 38% of patients and neuropsychiatric involvement in 23%. Additional symptom and biochemical test frequencies in Table 2.
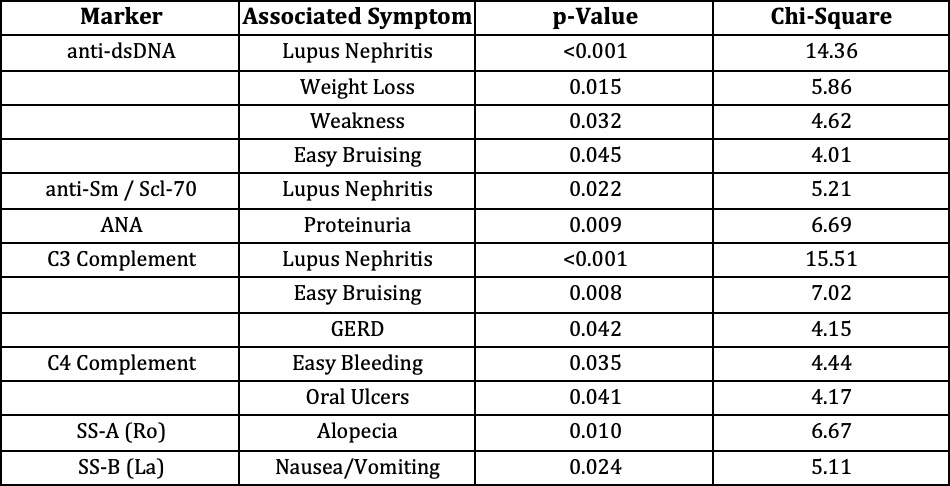
Lupus nephritis was associated with dsDNA antibodies (P < 0.001), low C3 (P < 0.001), and Sm/Scl-70 antibodies (P = .02) (Table 3). Low C4 was linked to the presence of oral ulcers (P = .04, Table 3). SS-A antibodies were associated with alopecia (P = 0.01, Table 3).
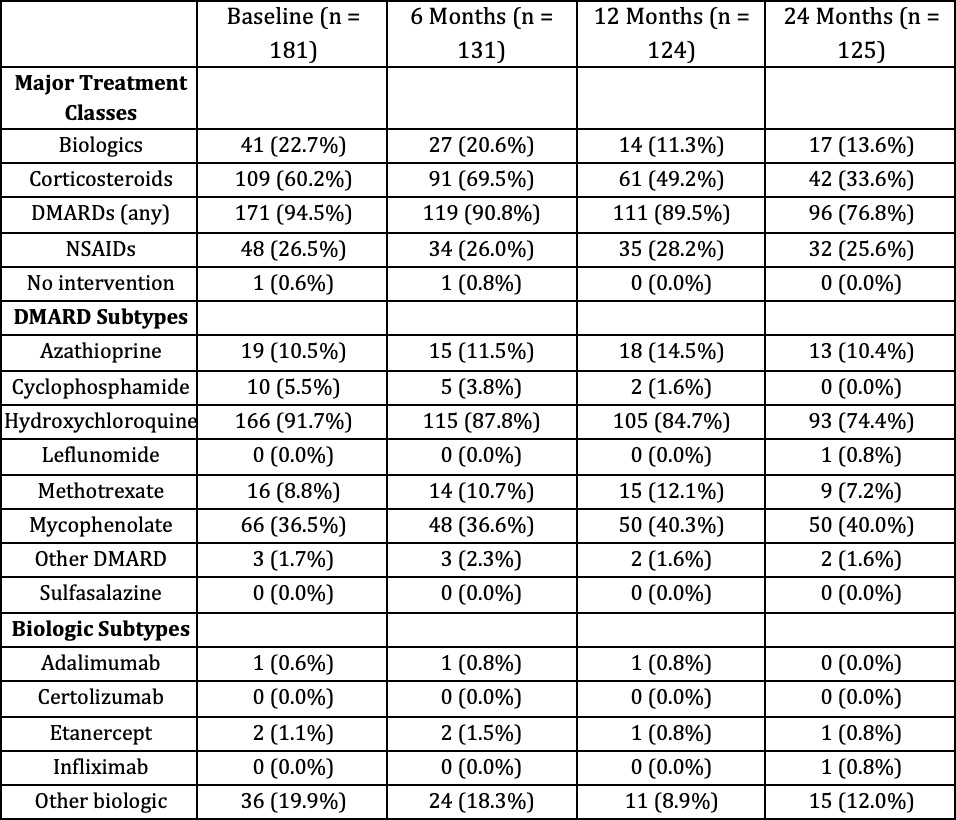
At 6 months, 23.7% of patients were symptom-free, increasing to 33.1% at 12 months and 44% at 24 months. However, those achieving complete remission including normalized biomarkers remained low, with 6.9% at 6 months, 4.0% at 12 months, and 7.2% at 24 months.
Conclusion: Symptom and biomarker presentation in Pediatric SLE is diverse, reinforcing the complex and heterogenous nature of the disease and the difficulty of treatment across various ages and disease severity. The correlation between immune markers and symptom appearance highlights the importance of early, consistent monitoring to evaluate disease trajectory and efficacy of treatment. Differences between pre- and post-pubertal presentations indicate the need for age-specific management rather than treating pediatric SLE as a monolith. Overall, these findings add important information and context to pediatric SLE to improve long-term outcomes and argue for greater personalized care.
Table 1. Patient Symptom and Biochemical Markers 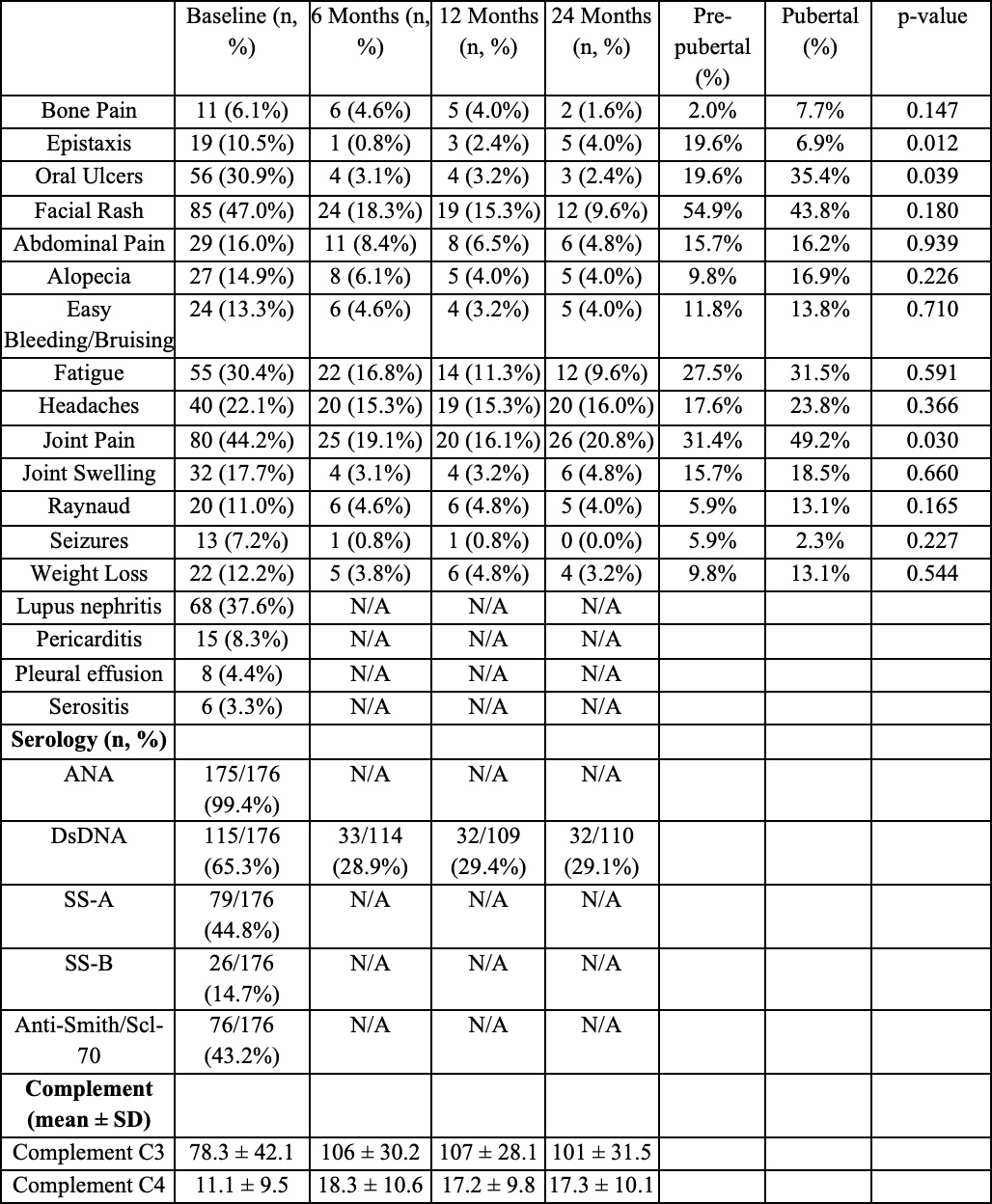
To cite this abstract in AMA style:
Campioli M, Widner J, Martinez A, Abdurrahman L, Lambert E, DeGuzman M. Rheumatological Biomarkers and Symptom Progression in Pediatric Systemic Lupus Erythematosus (SLE) [abstract]. Arthritis Rheumatol. 2026; 78 (suppl 3). https://acrabstracts.org/abstract/rheumatological-biomarkers-and-symptom-progression-in-pediatric-systemic-lupus-erythematosus-sle/. Accessed .« Back to 2026 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/rheumatological-biomarkers-and-symptom-progression-in-pediatric-systemic-lupus-erythematosus-sle/