Session Information
Date: Sunday, November 8, 2015
Title: Spondylarthropathies Psoriatic Arthritis - Pathogenesis, Etiology
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose:
The IL-17 axis has been identified as a crucial pathophysiological
pathway in spondyloarthritis (SpA). Targeting the IL-17 axis significantly
suppressed inflammation and halted bone and cartilage destruction in clinical
trials with secukinumab (anti-IL17A), brodalumab (anti-IL17RA), and ustekinumab
(anti-IL23/IL12p40) in ankylosing spondylitis and psoriatic arthritis. The
potential impact of IL-17A inhibition on new bone formation, the major form of
structural damage in SpA, remains unknown. Assessment of this feature requires
large patient numbers treated for an extended period and appropriate control
groups. Therefore, we aimed to assess the impact of anti-IL17A on new bone
formation in a validated animal model of SpA.
Methods:
6 weeks old, orchiectomized, HLA-B27/huβ2m tg rats (23-1×283-2) were immunized with 45 µg heat-inactivated M. tuberculosis/IFA.
Before the start of clinical symptoms, rats (n=6/group) were treated weekly with
an anti-mouse/rat IL-17A antibody or IgG2a isotype control at 15mg/kg i.p for 5
weeks. Clinical measurements included weight, clinical scores for spondylitis
and arthritis, and hind limb swelling (plethysmometry). After 6 weeks, rats
were sacrificed for skeletal analysis by mCT imaging and histology.
Results:
In the control group, spondylitis and arthritis were
observed in 100% of the rats at day 31 and day 19, respectively, after
immunization. In contrast, only 83% and 33% of the anti-IL-17A treated rats
developed spondylitis and arthritis at these time points. There was also a significant
delay in the mean appearance of spondylitis (day 28 vs day 14; p<0.05) and arthritis
(day 27 vs day 14; p<0.05) in treated versus control animals. Arthritis
severity was lower in the anti-IL-17A-treated group compared to the controls,
both by clinical scoring (p<0.05) and by plethysmometry (p<0.05). Quantitative
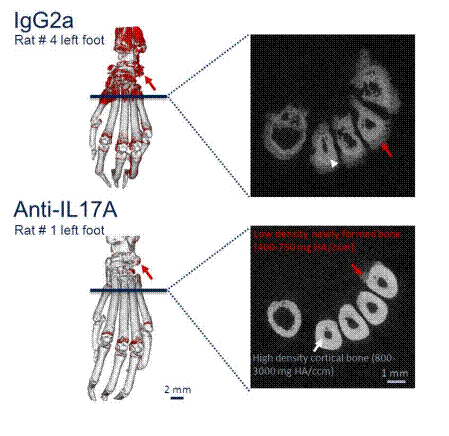
analysis of structural damage by mCT of foot and ankle joints (figure 1) showed a
significantly higher total bone volume in anti-IL-17A treated rats compared to
controls (17% more, p<0.05), suggesting decreased bone loss. Moreover, the
total volume of low density bone, reflecting newly formed bone, was significantly
lower in the anti-IL-17A treated rats than in controls (p<0.05). Histological
analysis confirmed a significant difference in structural damage in the
peripheral joints, especially with respect to periosteal new bone formation, which
was significantly less after anti-IL-17A treatment (p<0.01). In the axial
joints there was a tendency towards less inflammation, destruction and new bone
formation in the anti-IL-17A treated rats.
Conclusion:
IL-17A blockade significantly suppressed spondylitis and arthritis
in the M. tub-induced diseased HLA-B27 tg rat model of SpA. Moreover, mCT data and
histology indicated that IL-17A blockade also impacts structural damage,
including pathological new bone formation.
To cite this abstract in AMA style:
van Tok M, van Duivenvoorde L, Kramer I, Ingold P, Taurog J, Kolbinger F, Baeten D. Anti-IL-17A Treatment Blocks Inflammation, Destruction and New Bone Formation in Experimental Spondyloarthritis in HLA-B27 Transgenic Rats [abstract]. Arthritis Rheumatol. 2015; 67 (suppl 10). https://acrabstracts.org/abstract/anti-il-17a-treatment-blocks-inflammation-destruction-and-new-bone-formation-in-experimental-spondyloarthritis-in-hla-b27-transgenic-rats/. Accessed .« Back to 2015 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/anti-il-17a-treatment-blocks-inflammation-destruction-and-new-bone-formation-in-experimental-spondyloarthritis-in-hla-b27-transgenic-rats/