Session Information
Date: Sunday, November 8, 2015
Title: Fibromyalgia: Insights Into Diagnostic Criteria and Symptom Epidemiology
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: The American College of Rheumatology (ACR) 2010 preliminary criteria for the diagnosis of fibromyalgia requires ascertainment of pain extent and symptoms by physicians. The 2011 ÒsurveyÓ or ÒresearchÓ criteria modified the 2010 requirements by ascertaining criteria items entirely by patient self-report. Various concerns have been raised about potential problems with validity and reliability of the 2011 criteria. We used previously unreported patient data collected simultaneously from 514 patients in the ACR 2010 criteria study to compare physician based (MD) (2010) and patient based (PT) (2011) criteria.
Methods: From the 2010 study, we used data collected separately by physicians and patients for the widespread pain index (WPI), the symptom severity scale (SS), polysymptomatic distress scale (PSD) scale, and for fibromyalgia diagnosis using 2010 and 2011 study rules. A physician tender point count and determination of fibromyalgia by 1990 ACR criteria was also evaluated.
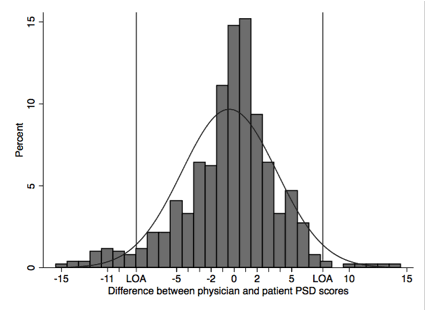
Results: The tender point count was strongly associated with the MD PSD scale (r=0.779) and PT PSD scale (r=0.702). Similar associations were noted with the MD WPI (r=0.751) and PT WPI (r=0.672). The area under the receiver operating curve (ROC) between tender point count and MD and PT diagnosis of fibromyalgia was 0.893 and 0.855. The MD and PT diagnostic agreement was substantial (83.4%, kappa = 0.67. PSD scores differed slightly: 12.3 (SD 7.7) for MD and 12.8 (SD 7.8) by PT, a difference of 0.42 units (p=0.213). The Bland-Altman 95% limits of agreement (LOA) for PSD was -8.5 and 7.7, with a standard error of the measurement of 2.9, and bias of -0.42 (Figure 1) [N.B. We will actually use Figure 2, below, for this ACR abstract].
Conclusion: MD and PT diagnosis and criteria items were strongly associated with tender points. Overall, there was good agreement in MD (2010) and PT (2011) fibromyalgia diagnosis and other measures. The low bias scores indicate consistent results for the physician and patient measures, but the large values for LOA indicate many widely discordant pairs. FM diagnostic agreement is greatest at high and low values of PSD, but becomes more uncertain as the 12-13 border line for diagnosis approaches There is acceptable agreement in diagnosis and PSD for research, but insufficient agreement for clinical decisions and diagnosis. If questionnaires are used to obtain clinical data for patient diagnosis, we recommend adjudication of symptom data by patient and physicians, as recommended by the 2010 ACR criteria.
Figure 1. Bland-Altman 95% Limits of Agreement (LOA) histogram. Mean difference (bias) is -0.42, Although PSD difference is close to 0, lack of agreement at individual physician-patient level is evident.
To cite this abstract in AMA style:
Wolfe F, Fitzcharles MA, Goldenberg D, Häuser W, Katz RS, Mease PJ, Russell A, Russell J, Walitt B. A Comparison of Physician Based and Patient Based Criteria for the Diagnosis of Fibromyalgia [abstract]. Arthritis Rheumatol. 2015; 67 (suppl 10). https://acrabstracts.org/abstract/a-comparison-of-physician-based-and-patient-based-criteria-for-the-diagnosis-of-fibromyalgia/. Accessed .« Back to 2015 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/a-comparison-of-physician-based-and-patient-based-criteria-for-the-diagnosis-of-fibromyalgia/